I hope this video will help you understand more about the how the list works in waiting for an organ.
Tag: heart transplant
Fears About Organ Donation
Survey Reveals Unfounded Fears About Organ Donation, US
Transplants / Organ Donations

A recent online survey of over 5,000 America adults found that misconceptions about the organ donation process are the most likely reasons for the gap between the number of people who would like to be donors and the number who actually register.
The main survey results are revealed in the annual report of the advocacy group Donate Life America. The report is titled “National Donor Designation Report Card, April 2009” and is the second annual report to detail the continued efforts to increase donor designations across America. The survey was conducted by Survey Sampling International for Donate Life America in partnership with Astellas Pharma US, Inc.
Most states in the US now have a straightforward scheme for licensed vehicle drivers to sign up to be organ donors: it only requires a signature and can be done when you apply for or renew your licence.
However, so far only 38 per cent of licensed drivers have signed up, and the survey suggests the reason could be fears and misconceptions about the organ donation process.
The survey showed that:
51 per cent of Americans wish to donate some or all of their organs and tissue.
Another 26 per cent are not sure.
58 per cent mistakenly believe that it is possible for a person to recover from brain death.
51 per cent incorrectly believe doctors may not try as hard to save a life, or aren’t convinced they will, when they know the patient is an organ donor.
44 per cent wrongly think that in the US there is a black market where people can buy and sell transplant organs and tissue.
23 per cent of people who reported being undecided, reluctant, or unwilling to donate their organs and tissue are not sure they would be accepted as donors. (The report said here that in reality, age and health status do not stop people from being potential donors because screening occurs before the organs are recovered for transplant).
The report says there are more than 100,000 Americans waiting for donor organs and tissue, and 18 die every day for lack of available organs.
There are also faces behind the numbers, and the report describes inspiring stories of donors and recipients, and the not so fortunate patient who died while waiting for an organ to be available.
Lorri was a 35-year-old mother who suffered a brain aneurism and was declared brain-dead but she had registered as a donor and “thanks to her compassionate gift seven people received lifesaving organ transplants, and countless more received the gifts of healing and renewal through tissue transplants”. The report describes her decision as giving peace to her family.
Seven year old Mikey can now do almost anything other boys his age can do, like ride his bike, roller skate and swim, thanks to a life saving liver transplant. But sadly baby Ryan, who was born with a dangerously enlarged heart, died at seven months while waiting for a new heart to become available.
Sara Pace Jones, who is chairwoman of Donate Life, told the New York Times that erroneous beliefs about organ donation could be a result of how it is shown on television dramas. She said some TV shows don’t have time in an hour to tell the whole story, and this can lead to inaccurate portrayals of how donation works.
“Many times I have seen a story unfold where the same physician treats the patient when admitted to the hospital, takes them to surgery, pronounces the patient dead, accesses the transplant list and does the organ recovery and transplant. But this is not how the donation process happens,” said Pace Jones.
But she stressed that the “doctor who is trying to save the life of the injured patient is not the same doctor who recovers organs for transplantation”.
Many people also don’t realize that the organizations that check the donor and patient registeries and co-ordinate the donations are separate from the hospitals that treat the recipients, she added.
Pace Jones said that people are reassured when they realize that “everything will be done to save their lives after an accident”, and when they understand that “the doctors who treat them have nothing to do with the transplantation process”.
Please take a moment and consider becoming an organ donor.
2015 Westfield Ma. Downtown Cultural Series
2015 Westfield Downtown Cultural Series
Saturday, October 17, 2015 2-4 p.m.
Lauren and I had the pleasure of meeting Joe, when we were in the hospital in Boston Ma. Lauren was recovering from her heart transplant and Joe was waiting for his new heart to arrive. A beautiful freindship began and continues……..
The trio will be performing as part of the downtown cultural series developed from a grant provided by MassDevelopment to bring attention to underutilized spaces in the downtown core area.
The show will take place at 55 ELM STREET from 2-4 pm. on Saturday, October 17th
The music we showcase is a collection of Latin Jazz, Modern jazz, traditional blues in the styles of BB King and Elmore James, as well as bringing a jazz twist on such artists as the Rolling Stones and Jimi Hendrix.
Join us for a great fall afternoon concert. Bring a chair, visit one of the local shops, grab some food and drink, and just have a good time with us
We will also be raising awareness for the group DONATE LIFE. Donate Life America is an organization that helps raise awareness and educate about the need for people to become organ and tissue donors. Without my heart transplant 18 months ago, this concert would not be possible. Please come down and talk to either Joe Whalen or fellow heart recipient Lauren Meizo of Chicopee to get information about how you can help.
Parent’s experience PTSD: Post Traumatic Stress Disorder
I came across this article written by Barb Roessner. For awhile I was starting to think I was just crazy or weak. PTSD : post traumatic stress disorder is real.
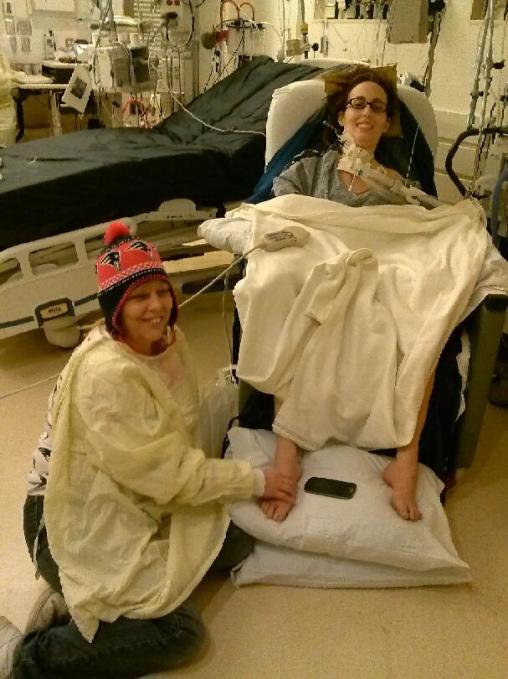
Living in the hospital with my daughter for close to almost a year and a half, was very hard. Always wondering and worrying with fear, no privacy and being closed in. All my freedom was taken away. After writing that sentence, all I feel is guilt. Oh my Lord, how my daughter must have felt. As a parent, I had to be the strong one for Lauren. I had to keep a smile on my face with tears from inside. When she was feeling down, I would do something crazy, like just break out in a dance just to try to make her laugh. She would say to me “your nuts mom”. Now when I think of it, I guess I was nuts. I was trying to cope with our situation also.
This picture was taken when we were watching a patriot’s football game. I was rubbing Lauren’s feet to make her more comfortable, and I was wearing my Patriot’s hat.
Living Life
PTSD is so real. There is not, one day that I do not have a flash back or memory though about what has happened. Some people say to me, you need to move forward. I am, but the memories do not go away. I guess I’m always afraid of going back.
To this day I still have a hard time going to a store, I can only stay in there for a short period of time, then I start to have anxiety, I do not like to be in close places anymore. Also, I have a hard time leaving my house. My house is my security. When I am home all is well. I know with time, it will get better but that saying “NO PLACE LIKE HOME” is so true.
Can Parents Experience PTSD from Their Child’s Heart Condition?
Written by: Barb Roessner
When most people think of post-traumatic stress disorder (PTSD), they imagine military veterans returning home from combat. Soldiers have been so exposed to human tragedy, their minds become conditioned to fight or flee, and surprising things—a firework exploding, someone dropping a book on the bus—could transport them back to the battlefield without warning.
People with PTSD may have trouble sleeping and struggle with constant anxiety. They feel like they’re on alert every second and struggle with memories of the traumatic events that are vivid enough to feel as if they’re happening to them again, according to the U.S. Department of Veterans Affairs.
But PTSD doesn’t just affect veterans. It can develop in individuals who have experienced any type of trauma—including parents who are watching their children struggle with a serious heart condition.
No, they are not in the midst of violence. And no, they are not bearing the medical burden of the heart condition. But the parents feel the agony of their child’s illness as if they are going through it themselves. They may always fear a meeting with a doctor, having heard the worst there before. Or they might forever associate their child crying in the night with a moment when the disease was especially trying.
Honestly, I think all families of kids with heart conditions have PTSD to varying degrees.
Think about it: the official definition of PTSD from the American Psychiatric Association doesn’t only include those who experience the trauma, but also those who witness it.
For families whose children have serious heart conditions, the parents’ stress level is high and rising all the time. We have cared for some families in which one or both of the parents sought treatment for PTSD. This usually happens during the waiting period: that time between being placed on the heart transplant list and actually getting a heart.
During that period, parents are on edge. They are constantly wondering when or if their child will receive a new heart in time. Then, they are faced with close calls that trigger their stress level to spike even higher, including:
Stroke
Kids with complex congenital heart conditions are at a higher risk of stroke. And not just 1 stroke, but they are at higher risk for recurrent strokes, according to a July 2012 study in the journal Annals of Neurology. Because their hearts are not functioning at their best, blockages can sometimes prevent blood from being pumped to the brain. Just like when anyone else has a stroke, this could cause serious disability or be life-threatening.
Cardiac arrest
Sudden cardiac arrest is a technical way of saying that the heart stops functioning. Congenital heart diseases—namely cardiomyopathy—are among the top reasons why children go into sudden cardiac arrest, according to a March 2012 study in the journal Pediatrics.
Extended waiting
Children listed for a heart transplant are more likely to pass away waiting than people waiting for any other type of solid organ transplant, according to a February 2009 study in the journal Circulation. As time goes by, the wait wears on parents, and it doesn’t get easier. That could be because one of the key risk factors for PTSD is feeling powerless, according to the U.S. Department of Veterans Affairs.
Then, there’s all the other complications that can happen. Some children have to have limbs amputated because of poor blood circulation. Some parents have literally watched their children stop breathing, turn blue and then had to entrust them to doctors and machines on faith that they’ll see them alive again.
For parents in any of these situations, when it’s a child—your child—you might as well be in the throes of a violent assault. The stress response is about the same.
I’ve only mentioned the medical complications. Let’s not forget about the strain on marriages, the financial burden that leads some families to bankruptcy and the issues that can arise with other children.
Why Addressing PTSD is So Important
The long-term issues of unchecked PTSD are serious, mainly because a prolonged fight or flight response is so taxing on the body.
Think about it: Your body is gearing up to protect itself from what it perceives to be an attack. The heart rate spikes to get more blood to your muscles, according to the National Alliance on Mental Illness.
Breathing speeds up, sometimes to the point of hyperventilating. Blood sugar spikes. If the body experiences this stress response too much, it could develop into long-term problems with high blood pressure.
This article is so true.
If you know someone who is in this situation please pass this on. They are not alone.
Reflections
This is a follow-up post from yesterday’s post.
September 16, 2015 Lauren spoke at the Chicopee Chamber of Commerce Breakfast as a guest speaker for Donate Life. It was a packed house. We were both nervous. Before Lauren became very sick, I had a business called Country Look Designs Gift Baskets. When I had my business, I was a member of this Chamber, it was a great way to meet other business people in the area. I did see some familiar faces,which was very nice.
When Lauren was giving her speech, she mention that she had a PA line in her neck (we called it her leash). This is Lauren with her PA Line in, before transplant .
This is a post Lauren wrote while waiting for her heart:
I need to have a “PA line” in my neck with two special medicines helping my heart beat stronger to be considered a 1A top of the list. Well I ended up getting the line in on that Friday and things were looking great until about 10:30 at night. My mom was rubbing my feet trying to relax me so I could fall asleep, then all of a sudden my heart rate started going up. Long story short, the ordeal went on until almost two in the morning. My room was filled with doctors and nurses from the ICU, which one of the doctors tried to jiggle the line. Once he had done that, all hell broke loose. I think there was a kink or something because after that a ton of the medicine released and my heart rate went up to 158. I had the x-ray machine in my room, ekgs done, the whole nine yards. My mom was crying because you could literally see my heart beating through my 101 lb body. All of a sudden my nurse told me they were ready to sedate me… and put the shock stickers on me.. yup, they were ready to jolt my ass! Scary! Instead they ended up pulling the line and for the rest of the weekend I was bumped down to a 1B statis. It was a stressful weekend because we were unsure if I was going to be able to get the “LEASH” back in my neck. I call it a leash as a joke because I only have about a 3 foot radius to walk around with it in… Just imagine being 22 and basically being bed bound for 10 days at a time while all your friends are progressing and having fun with there lives, actually imagine being any age and told you had to deal with this.
This picture was taken a couple of months after transplant.
My daughter Lauren endured every complication that could happen during her recovery. It was a long road for her, but for the most part she had that pretty smile on her face. She didn’t want to show me her fear, nor did I. Together we stayed strong, because we were going home someday.
This was the day we left the hospital, after 5 months of recovery. She never gave up, she still had the trac in and also her feeding tube. But we are going HOME !!!!!!!
When we walked through these doors in March of 2013, never thought we would be walking out May 2014.It was a long road, but I told my daughter we would be walking out together, with what we came for. Thank you GOD…

Blogging 201 is here
Today’s assignment: consider what you want to accomplish with your blog. Write down three concrete goals.
Starting this post, I really didn’t have to think that long and hard about why I write my blog. My daughter had a heart transplant on December 30, 2013
- Bringing awareness and education about organ donation.
Fact: 21 people die every day in the United States waiting for organs. Together we can lower that number by making that decision to become an organ donor. We were blessed, Lauren did receive her heart, but unfortunately many will not.
- To be able to reach out to more people so I can use my site as a forum for helping promote events, fundraiser and to help support different causes.
To name one http://www.hopeforcian.com/
- Double my number of followers
American Heart Association Halloween 5K walk
Traci Heath, from the American Heart Association ask me to help spread the word on a very important cause. Please pass this on, show your support. Sounds like a fun day for yourself and the family.
Traci Heath
Director at American Heart Association
Please help me get the word out about this Halloween 5k / walk. You can form a team, walk/run as an individual or with friends and family and bring the kids! Family oriented event on Halloween morning. Please wear your costumes! Face painting, games, Knight Productions DJ Entertainment and much more! Sponsors: Baystate Health / Health New England, Subway, Greylock Federal Credit Union, and WBRK!! Enjoy a fall foliage ride to the Berkshires on Halloween for this fun-filled event! Oct 31st @ BCC. http://www.berkshireheartwalk.org
Click on link below for more information
http://heartwalk.kintera.org/faf/home/default.asp?ievent=1131488
Information on Organ Donation
Are you an organ donor?
This could be one of your most important decision in your life you could make. I cannot think of a more beautiful tribute to your life, knowing if you could not be here in this world, you could help someone suffering, to live.
When I look at my daughter, there are times in my mind I try to picture the person who made the decision to be an organ donor. She saved Lauren’s life. We still do not know who the person was yet, but feel confident someday we will.
I believe this is a subject that most people don’t want to think about. Let’s face it, no one wants to think about their own death. I know I don’t. But, God forbid something was to happen to me. It would be a privilege to know that I could help others after I am gone. Take a moment to give this subject some though. If you have any questions about becoming an organ donor, I have posts that explains everything you need to know. Also you can go to Donate life.
If you could take a moment to take this poll, Lauren I would appreciate it.
Thank you
The Importance of a Transplant Social Worker
In this article, I want to focus on the importance of your social worker if you are living in a hospital with a life threatening medical condition.
When Lauren was admitted into the hospital, I felt like my world was turned upside down. I was so scared for my daughter. Looked around the room, so many monitors, machines so clinical and thinking this is my home now. I know my daughter was scared so I had to keep an upbeat persona to help her feel more at ease. Nurses were coming in and out, monitors were beeping, IV’s were being administered, so much, too much was happening.
At Brigham & Women’s all the cardiac patients have private rooms, that was a blessing. There was a couch in the room, so as I sat there with my husband just holding hands, my mind was going in a thousand directions. I knew he would have to go home in a couple of days to go to work, I had to dig deep to find the strength to figure out how the hell am I going to be able to live in a hospital room with my daughter, in a city I didn’t know, being 87 miles away from home. We had no idea how long we were going to be there. Days, weeks, months or a year. One thing I did know was, I was not leaving my daughter. We were in this together. From the outside people saw a different person, on the inside I was crying from fear.
We were meeting so many people, I would take their cards and on the back I would write little notes on them, like hair color, just something so that I could remember who they are. I didn’t want to be rude when they entered the room, if I couldn’t read their name badges.
There was one person we met that knew I wouldn’t forget her name, it was Kristen DeVoe, our social worker from the hospital. Kristen came into the room, introduced herself to us, then told us she was here to help us in anything we needed. She was not only there for Lauren, but she was there for me also.
Everyday, Kristen would come to our room to check on us, giving us emotional support, asking if we needed anything and I mean anything. Kristen became a very important confidant in my life. I found I could talk with her about anything. She also was a blessing when it came to taking care of medical paperwork, insurance forms basically anything. More important, when I just needed a hug or talk outside of Lauren’s room, Kristen was their for me. When Lauren wanted to talk, I would leave the room so she could have her one on one time also.
I wrote to Kristen and asked her if I could write a post about her and her job as a social worker. Even though we have been out of the hospital for a while now, I can still contact Kristen if I need to. Kristen’s answered “absolutely”. A social worker will not be your best friend, but during that time in the hospital, in my mind she was.
I would like to introduce you to,
Kristen DeVoe MSW, LICSW
Clinical Social Worker
Cardiac Transplant and Mechanical Circulatory Support
Brigham and Women’s Hospital
Some facts about my role…I’ll include my basic job description first:
· Work as part of a multidisciplinary team of physicians, nurses, dieticians and pharmacists.
· Provide comprehensive social work assessments as part of a pre-transplant or pre-ventricular assist device evaluation.
· Provide ongoing psychosocial and emotional support to patients and families before and after transplant and mechanical circulatory support.
· Facilitate a monthly support group for patients with mechanical circulatory support.
· Offer clinical opinions regarding the candidacy of potential transplant recipients at weekly selection committee meetings.
Boring, I know. So a lot of what I do is help patients and families get through the difficult process of waiting for a transplant. I provide support and counseling for patients before listing, while they are waiting and then after transplant. When I first meet a potential transplant patient I have to get to know them and make sure they have enough social support to get through the process successfully. I help patients manage anxiety and depression and basically serve as a source of support for them emotionally. I love my job. The relationships that I form with patients and families (like you and Lauren) are very important to me and I feel grateful that people allow me to share part of their journey. It truly is a privilege to work with the patients that I get to see and I’m constantly amazed by how much the human spirit can endure without breaking.
Kristen
Kristen DeVoe MSW, LICSW
Clinical Social Worker
Cardiac Transplant and Mechanical Circulatory Support
Brigham and Women’s Hospital
If you are living in a hospital, please take the support of your social worker. Dr.’s and nurses are very important components in your care, but also remember your social worker is as important also.
This post is dedicated to Kristen DeVoe and all the other social workers out there.
Lynne
Lauren will be speaking to the Chicopee Chamber of Commerce
Lauren has been invited to speak at a breakfast hosted by the Chicopee Chamber of Commerce on September 16th 2015.
Lauren’s last speaking event was in Boston, at the Harvard Medical School. She spoke about what it was like for a patient to live in the hospital for a lengthy period of time. The objective was to help inform the new and upcoming Doctors how she felt. Bedside manner, keeping her informed of her medical conditions and just letting them know she was a person not just a patient.
This speaking event with be about the importance of informing and educating on how to become an organ donor, and why people should sign up.
My thoughts are if we could save one life through a transplant, then we have helped.
Lynne